Achilles Tendinopathy - Managing Leg Pain
Nov. 28, 2023 #Heel Pain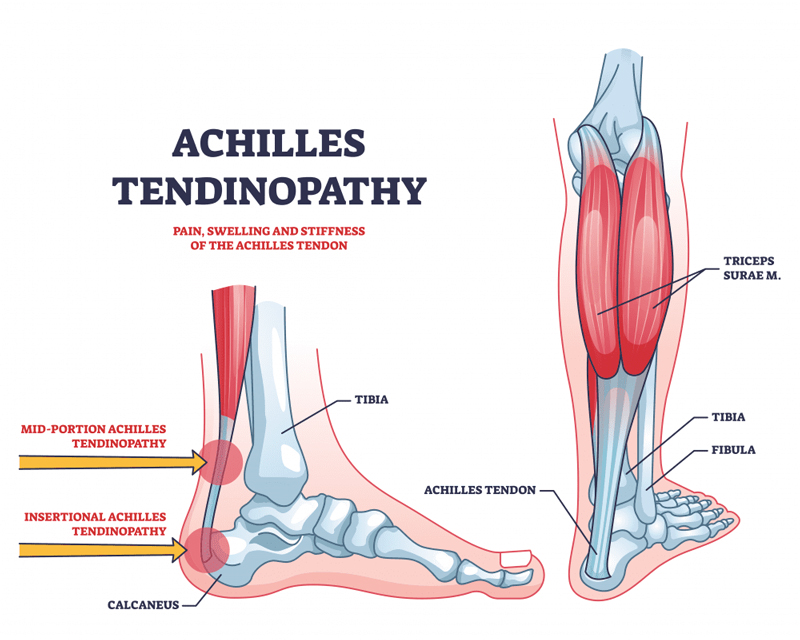
Achilles tendinopathy, a term encompassing conditions such as Achilles tendinitis and Achilles tendinosis, represents a prevalent and often debilitating issue affecting the Achilles tendon—the thick band of tissue connecting the calf muscles to the heel bone.
This article aims to provide a comprehensive exploration of Achilles tendinopathy, elucidating its definition, delving into the multifaceted causes, unraveling the varied symptoms, and shedding light on the diverse treatments available for individuals grappling with this challenging condition.
Defining Achilles Tendinopathy:
Achilles tendinopathy is a broad term used to describe disorders affecting the Achilles tendon, the largest and strongest tendon in the human body. Composed of fibrous tissue, the Achilles tendon plays a crucial role in facilitating movement, enabling activities such as walking, running and jumping. Achilles tendinopathy is not a single condition but rather an umbrella term that encompasses two primary stages: tendinitis and tendinosis.
Achilles Tendinitis: This refers to inflammation of the Achilles tendon. Inflammatory cells are present, indicating an acute response to injury or overuse.
Achilles Tendinosis: Unlike tendinitis, tendinosis involves chronic degeneration of the tendon without significant inflammation. It is characterized by the presence of microtears, collagen degeneration, and structural changes within the tendon.
Causes of Achilles Tendinopathy:
Several factors contribute to the development of Achilles tendinopathy, often involving a combination of intrinsic and extrinsic elements. Understanding these causative factors is essential for tailoring effective treatment plans. Common causes include:
Overuse and Repetitive Stress:
One of the primary culprits is overuse, particularly in activities that involve repetitive stress on the Achilles tendon. Runners, athletes engaging in jumping sports and individuals with sudden increases in activity levels may be at higher risk.
Improper Footwear:
Inadequate or inappropriate footwear, lacking proper support or causing abnormal stress on the Achilles tendon, can contribute to tendinopathy.
Biomechanical Factors:
Anomalies in foot mechanics, such as overpronation (excessive inward rolling of the foot) or flat feet, may increase the strain on the Achilles tendon.
Age and Gender:
Tendinopathy is more prevalent in individuals between the ages of 30 and 50. Additionally, males are generally at a higher risk than females.
Tight Calf Muscles:
Reduced flexibility and tightness in the calf muscles can place additional stress on the Achilles tendon, increasing susceptibility to injury.
Inadequate Warm-Up or Stretching:
Failing to warm up properly before engaging in physical activity or neglecting stretching exercises may predispose individuals to Achilles tendinopathy.
Medical Conditions:
Certain medical conditions, such as rheumatoid arthritis and gout, may contribute to the development of tendinopathy.
Symptoms of Achilles Tendinopathy:
Achilles tendinopathy manifests with a range of symptoms that can vary in intensity and duration. Common signs include:
Pain and Stiffness:
Pain is a hallmark symptom, often experienced along the back of the heel or above the heel bone. Stiffness may be prominent, especially in the morning or after periods of inactivity.
Swelling and Tenderness:
Swelling around the Achilles tendon and tenderness upon palpation are common features of tendinopathy.
Morning Pain and Stiffness:
Many individuals with Achilles tendinopathy report increased pain and stiffness in the morning, which may improve with movement.
Thickening of the Tendon:
In some cases, there may be a noticeable thickening of the Achilles tendon.
Difficulty with Foot Flexion:
Activities that involve pointing the toes downward (plantarflexion) can be particularly painful, making walking or climbing stairs challenging.
Treatments for Achilles Tendinopathy:
Effective management of Achilles tendinopathy involves a multifaceted approach addressing both symptoms and underlying causes. Treatment plans are often tailored to the severity of the condition and may include:
Rest and Activity Modification:
Adequate rest and modification of activities that exacerbate symptoms are essential components of treatment. This may involve temporary cessation of high-impact activities.
Ice Therapy:
Applying ice to the affected area can help reduce inflammation and alleviate pain. Ice packs or ice baths may be recommended.
Physical Therapy:
Physical therapy is a cornerstone of treatment, focusing on exercises to strengthen the calf muscles, improve flexibility and correct biomechanical issues.
Orthotics and Footwear Modification:
Custom orthotics or supportive footwear can help address biomechanical factors contributing to Achilles tendinopathy.
Calf Stretching Exercises:
Incorporating regular stretching exercises for the calf muscles can aid in improving flexibility and reducing strain on the Achilles tendon.
Nonsteroidal Anti-Inflammatory Drugs (NSAIDs):
NSAIDs may be recommended to alleviate pain and reduce inflammation. However, their use should be monitored and guided by a healthcare professional.
Eccentric Exercises:
Eccentric exercises, involving controlled lengthening of the Achilles tendon, have shown effectiveness in treating tendinopathy.
Shockwave Therapy:
Extracorporeal Shockwave Therapy (ESWT) involves the use of shockwaves to stimulate healing and may be considered in certain cases.
Corticosteroid Injections (in selective cases):
Injections of corticosteroids into the affected area may be recommended for short-term relief of inflammation and pain. However, repeated use should be cautious due to potential side effects.
Surgical Intervention (in severe cases):
Surgery is considered only in cases of severe or persistent Achilles tendinopathy that does not respond to conservative treatments. Procedures may involve removing damaged tissue or repairing the tendon.
Conclusion: Navigating the Road to Recovery:
Achilles tendinopathy poses a unique set of challenges, requiring a comprehensive and personalized approach to achieve optimal outcomes. Timely intervention, a commitment to rehabilitation exercises, and addressing contributing factors are vital components of the recovery journey.
Individuals experiencing symptoms of Achilles tendinopathy should seek prompt medical attention to receive an accurate diagnosis and initiate a tailored treatment plan. With the right interventions and a proactive approach to preventive measures, many individuals can overcome Achilles tendinopathy and resume their normal activities with reduced pain and improved function.
Frequently Asked Questions (FAQs) on Achilles Tendinopathy
1. What is Achilles Tendinopathy?
Achilles Tendinopathy is a term encompassing conditions such as Achilles tendinitis and tendinosis, representing disorders affecting the Achilles tendon. It involves inflammation (tendinitis) or chronic degeneration (tendinosis) of the Achilles tendon, causing pain and stiffness.
2. What Causes Achilles Tendinopathy?
Achilles tendinopathy can result from various factors, including overuse, improper footwear, biomechanical issues (such as flat feet or overpronation), tight calf muscles, age, gender and medical conditions like arthritis.
3. Who is at Risk for Developing Achilles Tendinopathy?
Individuals engaged in activities with repetitive stress on the Achilles tendon, such as runners and athletes, may be at higher risk. Factors like age, gender and biomechanical issues can also contribute to susceptibility.
4. What are the Common Symptoms of Achilles Tendinopathy?
Symptoms include pain and stiffness along the back of the heel, swelling, tenderness, morning pain and stiffness, thickening of the tendon, and difficulty with foot flexion, especially during activities like walking or climbing stairs.
5. How is Achilles Tendinopathy Diagnosed?
Diagnosis involves a thorough physical examination, medical history review and imaging studies (X-rays and MRI), to rule out other potential causes of heel pain. A healthcare professional can provide an accurate diagnosis.
6. What Treatments are Available for Achilles Tendinopathy?
Treatment includes rest, activity modification, ice therapy, physical therapy (exercises to strengthen and stretch muscles), orthotics or supportive footwear, anti-inflammatory medications, eccentric exercises, shockwave therapy, corticosteroid injections (in selective cases) and surgery (in severe cases).
7. Can I Continue Physical Activities if I Have Achilles Tendinopathy?
Activity modification is usually recommended, meaning temporary cessation or modification of activities that worsen symptoms. Low-impact exercises and proper warm-up routines may be suggested. Consult with a healthcare professional for personalized advice.
8. How Long Does Recovery from Achilles Tendinopathy Take?
Recovery time varies based on the severity of the condition, adherence to treatment and individual factors. With appropriate interventions, many individuals experience significant improvement within a few weeks to months.
9. Can Achilles Tendinopathy Recur?
Recurrence is possible, especially if contributing factors are not addressed. Preventive measures, including calf stretching, strengthening exercises and proper footwear, can help minimize the risk of recurrence.
10. Should I Consider Surgery for Achilles Tendinopathy?
Surgery is reserved for severe or persistent cases that do not respond to conservative treatments. It may involve removing damaged tissue or repairing the tendon. Surgical options should be discussed with a healthcare professional.
11. Can I Use Corticosteroid Injections for Long-Term Relief?
Corticosteroid injections may provide short-term relief but are generally not recommended for long-term use due to potential side effects. Their use should be monitored and guided by a healthcare professional.



COMMENTS