Pulmonary Hypertension - The Bridge between Breath and Blood Pressure
Dec. 1, 2023 #Hypertension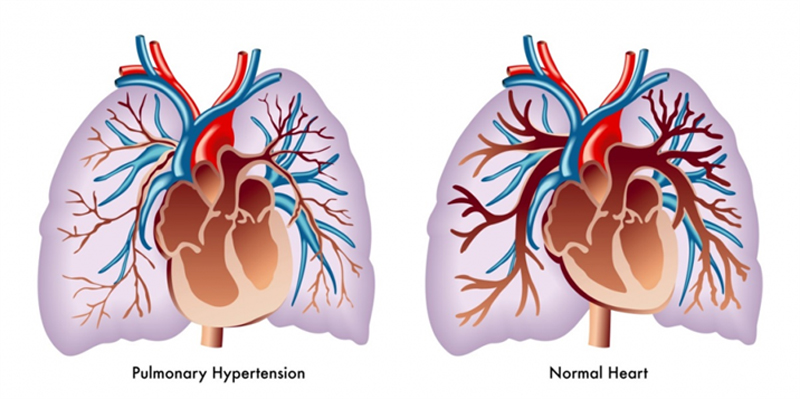
Pulmonary hypertension (PH) is a medical condition characterized by elevated blood pressure within the pulmonary arteries, which supply blood to the lungs. This condition involves the narrowing, stiffening, or blockage of these arteries, leading to increased resistance to blood flow.
As a result, the right side of the heart must work harder to pump blood into the lungs, potentially causing strain and adverse effects on heart function. Understanding the definition, causes, symptoms, and available treatments for pulmonary hypertension is crucial for effective management and improved quality of life.
Defining Pulmonary Hypertension:
Pulmonary hypertension is a complex and progressive condition that affects the pulmonary arteries, responsible for carrying oxygen-depleted blood from the heart to the lungs. In a normal circulatory system, these arteries have low pressure.
However, in pulmonary hypertension, increased pressure within these vessels makes it more challenging for the heart to pump blood through the lungs. The condition is categorized into five groups based on the underlying causes and characteristics.
Causes of Pulmonary Hypertension:
Several factors can contribute to the development of pulmonary hypertension, and understanding the underlying cause is essential for appropriate management. Common causes include:
Idiopathic Pulmonary Arterial Hypertension (IPAH):
In some cases, the cause remains unknown, leading to idiopathic pulmonary arterial hypertension. This form is often hereditary and may involve genetic factors.
Secondary Pulmonary Hypertension:
Underlying medical conditions such as heart diseases, lung diseases (chronic obstructive pulmonary disease or interstitial lung disease), blood clots in the lungs (pulmonary embolism), and sleep apnea can lead to secondary pulmonary hypertension.
Connective Tissue Disorders:
Conditions like scleroderma, lupus, and rheumatoid arthritis can affect the connective tissues of the lungs, contributing to pulmonary hypertension.
Congenital Heart Diseases:
Some individuals may develop pulmonary hypertension due to congenital heart defects that affect the normal flow of blood through the heart and lungs.
Left Heart Diseases:
Conditions affecting the left side of the heart, such as heart failure or valvular diseases, can result in increased pressure in the pulmonary arteries.
Symptoms of Pulmonary Hypertension:
The symptoms of pulmonary hypertension can vary depending on the severity of the condition and its underlying cause. Common symptoms include:
Shortness of Breath (Dyspnea):
Difficulty breathing, especially during physical activity, is a hallmark symptom of pulmonary hypertension.
Fatigue:
Chronic fatigue and weakness are common due to the increased workload on the heart.
Chest Pain:
Individuals with pulmonary hypertension may experience chest pain or discomfort, especially during exertion.
Dizziness or Fainting (Syncope):
Reduced blood flow to the brain can lead to dizziness or fainting spells.
Swelling (Edema):
Swelling in the ankles and legs may occur due to fluid retention.
Cyanosis:
Bluish discoloration of the lips and skin, known as cyanosis, can result from decreased oxygen levels in the blood.
Treatment Options for Pulmonary Hypertension:
Managing pulmonary hypertension involves addressing the underlying cause and alleviating symptoms to improve quality of life. Treatment options include:
Medications:
Various medications are prescribed to dilate blood vessels, reduce blood clot formation and improve heart function. These may include vasodilators, anticoagulants, and medications targeting specific pathways involved in pulmonary hypertension.
Oxygen Therapy:
Supplemental oxygen is often prescribed to improve oxygen levels in the blood and relieve symptoms of breathlessness.
Pulmonary Rehabilitation:
Pulmonary rehabilitation programs focus on exercise, education, and support to help individuals manage their symptoms and improve physical endurance.
Surgery or Interventional Procedures:
In some cases, surgical interventions or procedures such as lung transplantation, atrial septostomy (creating an opening in the atrial septum), or balloon pulmonary angioplasty may be considered.
Diuretics:
Diuretics may be prescribed to manage fluid retention and reduce swelling.
Lifestyle Modifications:
Lifestyle changes, including maintaining a healthy diet, staying physically active within individual limits, and avoiding smoking, can contribute to overall well-being.
Continuous Monitoring:
Regular monitoring and follow-up with healthcare providers are crucial to adjust treatment plans based on the individual's response and the progression of pulmonary hypertension.
Prognosis and Outlook:
The prognosis for pulmonary hypertension varies based on the underlying cause, the severity of the condition at the time of diagnosis, and the effectiveness of treatment. Early diagnosis and appropriate management can improve symptoms and slow the progression of the disease. However, pulmonary hypertension can be a serious and life-limiting condition in some cases.
Conclusion:
Pulmonary hypertension poses unique challenges due to its impact on the circulatory system, affecting both the heart and lungs. Timely diagnosis, comprehensive evaluation of the underlying causes, and a multidisciplinary approach to treatment are essential for individuals facing this condition. With advancements in medical therapies and ongoing research, there is hope for improved outcomes and enhanced quality of life for those living with pulmonary hypertension. As with any medical condition, collaboration with healthcare professionals ensures a tailored and effective approach to managing pulmonary hypertension.






COMMENTS