Greater Trochanteric Pain Syndrome
Nov. 30, 2023 #Back Pain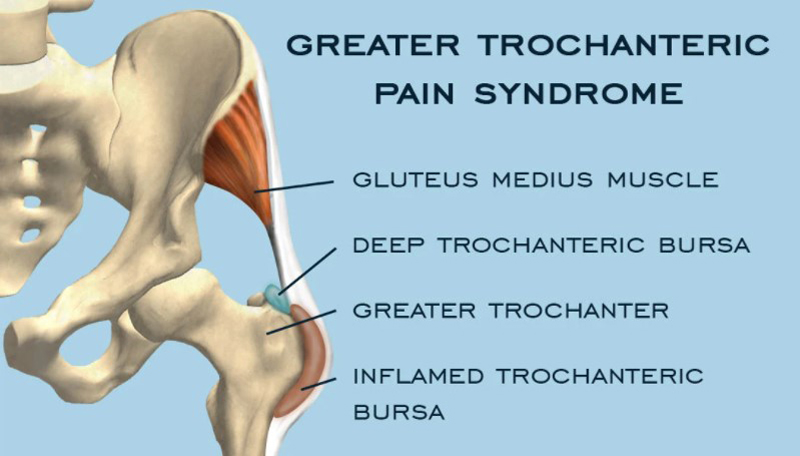
Greater Trochanteric Pain Syndrome (GTPS) is a condition characterized by pain and tenderness over the greater trochanter, a bony prominence on the femur (thigh bone). This syndrome encompasses a spectrum of disorders affecting the hip and lateral pelvic region.
GTPS is a common cause of lateral hip pain and is often associated with inflammation or injury to the tendons and bursa surrounding the greater trochanter. Understanding the causes, symptoms, and available treatments is crucial for effective management of Greater Trochanteric Pain Syndrome.
Defining Greater Trochanteric Pain Syndrome:
The greater trochanter is a bony prominence on the outer side of the femur, serving as an attachment point for various muscles and tendons. GTPS involves pain and tenderness in this area, often associated with inflammation of the tendons (tendinitis) or bursa (bursitis). The condition is multifactorial, and its exact cause can vary among individuals.
Causes of Greater Trochanteric Pain Syndrome:
Several factors contribute to the development of GTPS:
Tendon Abnormalities:
Tendinitis involving the tendons that attach to the greater trochanter, such as the gluteus medius or gluteus minimus tendons, is a common cause of GTPS.
Bursitis:
Inflammation of the trochanteric bursa, a fluid-filled sac that provides cushioning between tendons and bones, can contribute to GTPS.
Repetitive Stress or Overuse:
Activities that involve repetitive movements or prolonged stress on the hip, such as running or climbing stairs, can lead to irritation and inflammation of the tendons and bursa.
Hip Muscle Weakness or Imbalance:
Weakness or imbalance in the muscles around the hip, particularly the gluteal muscles, can contribute to abnormal stress on the greater trochanter and predispose individuals to GTPS.
Trauma or Injury:
Direct trauma to the hip or a fall onto the side of the hip can cause damage to the tendons and bursa, leading to GTPS.
Bone Abnormalities:
Structural issues or abnormalities in the hip joint, such as hip dysplasia or abnormalities in the shape of the femur, may contribute to GTPS.
Systemic Diseases:
Conditions like rheumatoid arthritis or systemic lupus erythematosus may contribute to inflammation around the greater trochanter.
Symptoms of Greater Trochanteric Pain Syndrome:
The hallmark symptom of GTPS is lateral hip pain, often described as a deep ache or sharp pain. Other common symptoms include:
Tenderness Over Greater Trochanter:
Palpation of the greater trochanter elicits tenderness.
Pain with Movement:
Pain is often aggravated by activities that involve hip movement, such as walking, climbing stairs, or lying on the affected side.
Radiating Pain:
Pain may radiate down the outer thigh or buttock.
Stiffness:
Stiffness or limited range of motion in the hip joint may be present.
Pain at Rest:
Some individuals may experience pain even at rest, especially when lying on the affected side.
Treatment Options for Greater Trochanteric Pain Syndrome:
Effective management of GTPS involves a multifaceted approach addressing the underlying causes and relieving symptoms. Treatment options include:
Rest and Activity Modification:
Resting the affected hip and modifying activities that exacerbate symptoms can help reduce irritation and promote healing.
Physical Therapy:
Physical therapy is a cornerstone of GTPS management. Therapeutic exercises focus on strengthening hip muscles, improving flexibility and correcting biomechanical issues contributing to the syndrome.
Anti-Inflammatory Medications:
Nonsteroidal anti-inflammatory drugs (NSAIDs) may be prescribed to reduce inflammation and alleviate pain.
Corticosteroid Injections:
In cases of significant inflammation, corticosteroid injections into the trochanteric bursa may provide short-term relief.
Activity Modification and Ergonomic Changes:
Modifying activities and making ergonomic changes, such as adjusting footwear or using assistive devices, can alleviate stress on the hip.
Ice and Heat Therapy:
Applying ice or heat to the affected area may help reduce pain and inflammation.
Orthotics:
In some cases, the use of orthotic devices or shoe inserts may help correct gait abnormalities and alleviate stress on the hip.
Weight Management:
Maintaining a healthy weight is important for reducing stress on the hip joints and preventing exacerbation of symptoms.
Ultrasound-Guided Interventions:
Advanced interventions, such as ultrasound-guided needle procedures, may be considered for targeted treatment of affected tendons or bursa.
Surgical Intervention:
In refractory cases, surgical intervention may be considered. This may involve debridement of damaged tissue, repair of tendons or other procedures aimed at addressing structural issues.
Prognosis and Outlook:
The prognosis for GTPS is generally favorable with appropriate treatment. Most individuals experience relief from symptoms with conservative measures, including physical therapy and lifestyle modifications. Surgical intervention is typically reserved for cases resistant to conservative management.
Conclusion:
Greater Trochanteric Pain Syndrome poses a significant challenge for those experiencing hip pain and discomfort. Seeking timely medical attention, a comprehensive diagnosis and a tailored treatment plan are essential for effective management.
Frequently Asked Questions (FAQs)
1. What is Greater Trochanteric Pain Syndrome (GTPS)?
GTPS is a condition characterized by pain and tenderness over the greater trochanter, a bony prominence on the femur. It often involves inflammation or injury to the tendons and bursa around this area.
2. What causes GTPS?
GTPS can result from various factors, including tendon abnormalities, bursitis, repetitive stress or overuse, hip muscle weakness, trauma or injury, bone abnormalities and systemic diseases.
3. What are the common symptoms of GTPS?
The primary symptom is lateral hip pain, described as a deep ache or sharp pain. Tenderness over the greater trochanter, pain with movement, radiating pain, stiffness and pain at rest are common symptoms.
4. How is GTPS diagnosed?
Diagnosis involves a thorough medical history review, physical examination and imaging studies such as X-rays or MRI to assess the hip joint and surrounding structures.
5. Can GTPS be mistaken for other hip conditions?
Yes, GTPS symptoms can overlap with other hip conditions. Proper diagnosis is crucial to differentiate GTPS from conditions like hip osteoarthritis or labral tears.
6. What contributes to the development of GTPS?
Contributing factors include repetitive movements, muscle weakness, trauma, structural abnormalities and systemic diseases. Identifying and addressing these factors are crucial for effective management.
7. How is GTPS treated?
Treatment options include rest, physical therapy, anti-inflammatory medications, corticosteroid injections, activity modification, orthotics, weight management, and, in severe cases, surgical intervention.
8. Can GTPS be managed at home?
Mild cases may be managed at home with rest, over-the-counter pain medications, ice or heat therapy and activity modification. However, consultation with a healthcare professional is recommended for proper guidance.
9. Is physical therapy beneficial for GTPS?
Yes, physical therapy is a key component of GTPS management. Therapeutic exercises focus on strengthening hip muscles, improving flexibility and correcting biomechanical issues.
10. Are there lifestyle changes that can help with GTPS?
-Yes, lifestyle changes such as weight management, ergonomic adjustments and orthotic use can help alleviate stress on the hip joint and improve symptoms.
11. When is surgical intervention considered for GTPS?
-Surgical intervention is considered in refractory cases where conservative measures are ineffective. Procedures may involve debridement, tendon repair, or addressing structural issues contributing to GTPS.
12. Can GTPS recur after treatment?
-While many individuals experience relief with treatment, GTPS can recur, especially if underlying factors are not addressed. Maintaining a healthy lifestyle and addressing contributing factors are essential for prevention.
13. Can GTPS affect daily activities?
-Yes, GTPS can impact daily activities due to pain and a limited range of motion. With effective management, most individuals can resume normal activities.
14. How long does it take to recover from GTPS?
-Recovery time varies, and mild cases may resolve with conservative measures in a few weeks. Severe cases or those requiring surgery may have a more extended recovery period.
15. Where can I find support for GTPS?
-Support can be found through healthcare professionals specializing in orthopedics or pain management, physical therapists and online resources. Connecting with others who have experienced GTPS can provide valuable insights and support.






COMMENTS