Patellofemoral Pain Syndrome - Treating Knee Pain
Nov. 28, 2023 #Back Pain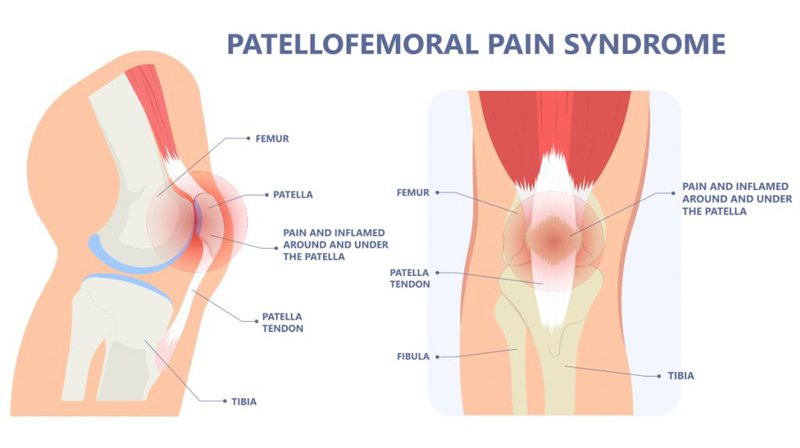
Patellofemoral Pain Syndrome (PFPS) is a common orthopedic condition characterized by pain around or behind the patella (kneecap). Often referred to as "runner's knee," PFPS is not exclusive to athletes and can affect individuals of all activity levels.
This article explores the intricacies of Patellofemoral Pain Syndrome, delving into its definition, causes, symptoms and the array of treatments available to alleviate the discomfort associated with this prevalent knee ailment.
Defining Patellofemoral Pain Syndrome:
Patellofemoral Pain Syndrome originates from issues within the patellofemoral joint, where the patella glides over the femur. The friction or misalignment of the patella within the femoral groove can result in pain and discomfort. PFPS is often considered an umbrella term, encompassing a spectrum of conditions that cause anterior knee pain. It commonly arises from overuse, muscle imbalances and misalignment of the patella, leading to abnormal tracking and increased pressure on the joint surfaces.
Causes of Patellofemoral Pain Syndrome:
Several factors contribute to the development of Patellofemoral Pain Syndrome, and a multifaceted approach is often required to pinpoint the precise cause. Some key factors include:
Muscle Imbalances:
Weakness or imbalance in the muscles surrounding the knee, particularly the quadriceps and hamstrings, can alter the patellar tracking and contribute to PFPS.
Overuse and Excessive Load:
Repetitive activities, especially those involving high-impact or excessive load-bearing on the knee joint, can lead to irritation and inflammation, a common precursor to PFPS.
Malalignment of the Patella:
Anatomical variations, such as a misaligned patella or abnormalities in the structure of the lower limb, can contribute to the onset of PFPS.
Trauma or Injury:
Direct trauma to the knee, such as a fall or blow to the kneecap, can trigger PFPS. Additionally, sudden changes in activity levels or improper training techniques may contribute to injury.
Flat Feet or Overpronation:
Individuals with flat feet or those who overpronate (excessive inward rolling of the foot) may be more prone to PFPS due to altered biomechanics and increased stress on the patellofemoral joint.
Symptoms of Patellofemoral Pain Syndrome(PFPS):
The hallmark symptom of PFPS is anterior knee pain, typically felt around or behind the kneecap. The pain may be exacerbated by activities that involve bending the knee, such as squatting, running or climbing stairs. Other common symptoms include:
Pain During or After Activity:
Discomfort often intensifies during or after engaging in physical activities, particularly those that stress the patellofemoral joint.
Pain with Prolonged Sitting:
Individuals with PFPS may experience increased pain after sitting for extended periods, as this can exacerbate patellar compression.
Pain Descending Stairs:
Descending stairs or hills can be particularly painful for those with PFPS due to increased load on the patellofemoral joint.
Grinding Sensation:
Some individuals may report a grinding or popping sensation in the knee when moving it.
Swelling or Tenderness:
Swelling and tenderness around the patella may be present, especially after prolonged activity.
Treatments for Patellofemoral Pain Syndrome:
Addressing Patellofemoral Pain Syndrome often involves a combination of conservative treatments aimed at relieving symptoms and addressing underlying causes. Some common interventions include:
Physical Therapy:
Tailored exercises to strengthen the quadriceps, hamstrings, and hip muscles help improve patellar tracking and address muscle imbalances.
Activity Modification:
Temporarily reducing or modifying activities that exacerbate symptoms can facilitate healing and prevent further irritation.
Orthotics or Shoe Inserts:
For individuals with flat feet or overpronation, orthotics or shoe inserts can help correct biomechanical issues and reduce stress on the patellofemoral joint.
Bracing or Taping:
Patellar braces or kinesiology taping may provide support and help align the patella, reducing pain during movement.
Anti-Inflammatory Medications:
Nonsteroidal anti-inflammatory drugs (NSAIDs) can be used to alleviate pain and reduce inflammation.
RICE Protocol:
Rest, Ice, Compression and Elevation (RICE) can be effective in managing acute symptoms and promoting recovery.
Corticosteroid Injections:
In some cases, corticosteroid injections may be considered to reduce inflammation and alleviate pain.
Surgical Interventions (in rare cases):
Surgical options, such as arthroscopy, may be considered for persistent cases that do not respond to conservative treatments. However, surgery is typically reserved for cases with structural abnormalities.
Future Outlook and Preventive Measures:
The outlook for individuals with Patellofemoral Pain Syndrome is generally positive with appropriate treatment. However, the recurrence of symptoms is possible, emphasizing the importance of preventive measures. Incorporating proper warm-up and cool-down routines, maintaining balanced muscle strength, and gradually increasing activity levels can help prevent the onset or recurrence of PFPS. Moreover, seeking prompt medical attention for any knee pain and addressing contributing factors, such as biomechanical issues or overuse, can contribute to long-term joint health.
In conclusion, Patellofemoral Pain Syndrome presents a common challenge for individuals of various activity levels, impacting their quality of life. A comprehensive approach that addresses both symptoms and underlying causes is crucial for effective management. With the right interventions, including physical therapy, activity modification, and conservative treatments, individuals can often return to their regular activities and enjoy a pain-free lifestyle.
Frequently Asked Questions (FAQs)
1. What is Patellofemoral Pain Syndrome (PFPS)?
Patellofemoral Pain Syndrome, often referred to as "runner's knee," is a common orthopedic condition characterized by pain around or behind the kneecap (patella). It arises from issues within the patellofemoral joint, involving the interaction between the patella and the femur.
2. What are the Causes of PFPS?
PFPS can be caused by a variety of factors, including muscle imbalances, overuse, malalignment of the patella, trauma or injury and structural issues such as flat feet or overpronation.
3. Who is at Risk for Developing PFPS?
PFPS can affect individuals of all ages and activity levels. However, those engaged in activities that involve repetitive knee movements, such as running, jumping, or squatting, may be at a higher risk. Additionally, individuals with muscle imbalances, flat feet, or previous knee injuries may be more prone to PFPS.
4. What are the Common Symptoms of PFPS?
The hallmark symptom is anterior knee pain, often felt around or behind the kneecap. Pain is typically exacerbated by activities such as running, squatting, or descending stairs. Some individuals may also experience a grinding sensation, swelling or tenderness around the patella.
5. How is PFPS Diagnosed?
PFPS is often diagnosed through a thorough physical examination, medical history review, and imaging studies, such as X-rays or MRI, to rule out other potential causes of knee pain.
6. What Treatments are Available for PFPS?
Treatment for PFPS is typically conservative and may include physical therapy, activity modification, orthotics or shoe inserts, bracing or taping, anti-inflammatory medications, the RICE protocol (Rest, Ice, Compression, Elevation), and in some cases, corticosteroid injections. Surgical interventions are rare and considered only for persistent cases.
7. Can PFPS be Prevented?
Yes, several preventive measures can help reduce the risk of developing PFPS. These include maintaining balanced muscle strength, incorporating proper warm-up and cool-down routines, gradually increasing activity levels, and addressing any biomechanical issues or overuse promptly.
8. Should I Continue Physical Activity if I Have PFPS?
In most cases, it is advisable to modify activities rather than completely cease them. Low-impact exercises, such as swimming or cycling, may be substituted for high-impact activities. It's essential to consult with a healthcare professional for personalized advice based on the severity of symptoms.
9. How Long Does it Take to Recover from PFPS?
The recovery time for PFPS varies based on individual factors, the severity of symptoms and the effectiveness of treatment. With appropriate and consistent treatment, many individuals experience significant improvement within a few weeks to months.
10. Can PFPS Recur After Recovery?
Recurrence of PFPS is possible, especially if contributing factors, such as muscle imbalances or overuse, are not addressed. Maintaining a balanced exercise routine, incorporating preventive measures, and seeking prompt medical attention for any recurrence can help minimize the risk of persistent issues.
Remember, this FAQ is for informational purposes only and should not replace professional medical advice. If you suspect you have PFPS or are experiencing knee pain, consult with a healthcare professional for an accurate diagnosis and appropriate treatment plan.






COMMENTS